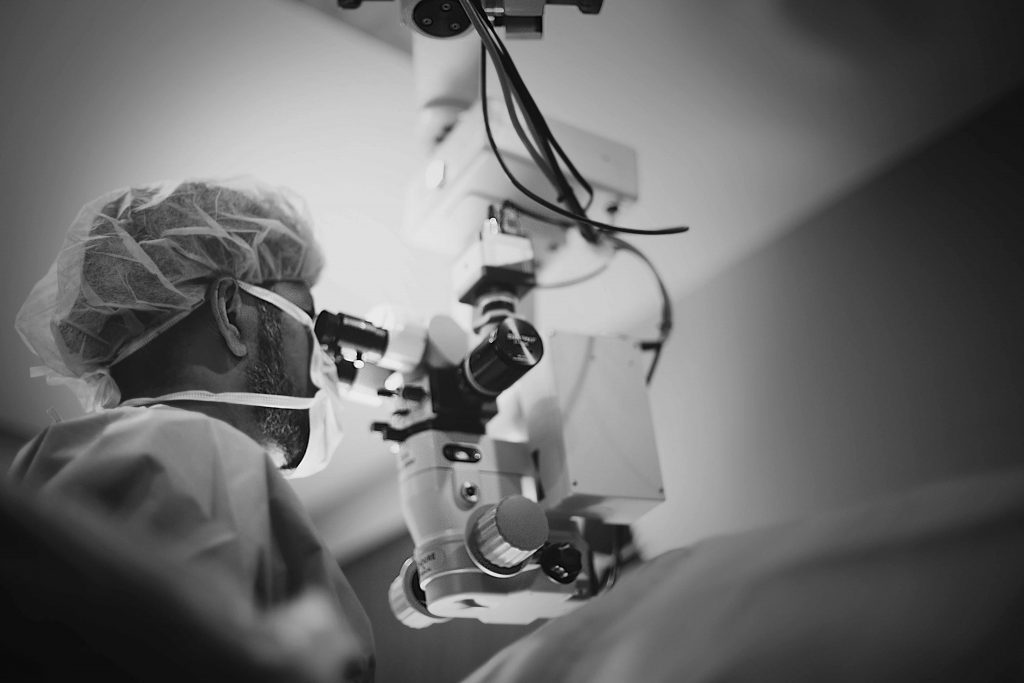
If you’re experiencing cloudy vision, glare or difficulty reading, cataracts may be the reason. Milan Eye Center offers advanced cataract surgery in Atlanta performed by board-certified, fellowship-trained surgeons. Using both traditional and laser-assisted techniques, we tailor each procedure to your visual goals and lifestyle.
At Milan Eye Center, we’re proud to be known as the “Doctor’s Doctors.” Local physicians and medical professionals have trusted our surgeons for their own eye care — and that of their families. Our board-certified, fellowship-trained surgeons are respected throughout the Atlanta medical community for delivering exceptional results.
We offer both traditional and laser-assisted cataract surgery using the Ziemer FEMTO LDV Z8 laser, an FDA-approved technology that allows our surgeons to perform bladeless, ultra-precise incisions. This leads to greater safety, more predictable results, and a more personalized surgical experience.
Our team frequently treats patients who have been turned away elsewhere due to complicating factors or high-risk conditions. Whether it’s a dense cataract, previous eye surgery or unique anatomy, our surgeons have the expertise and tools to take on challenging cases.
With eight locations and fully accredited surgical centers, Milan Eye Center makes high-quality care easy to access. Each facility is equipped with state-of-the-art diagnostic and surgical technology and a team dedicated to your comfort every step of the way.

Cataracts are cloudy lenses within our eyes. As we age, the proteins in our lenses become more opaque, causing cloudiness. Cataracts are very common, affecting roughly 60% of people over the age of 60. (Watch Video)
Many develop cataracts gradually due to the natural aging process. Still, cataracts can develop quicker from exposure to UV light, smoking, diabetes, eye injury, or the use of certain medications, such as steroids.
Many patients consider poor vision an inevitable fact of aging. However, cataract eye surgery has become an incredibly sophisticated and safe procedure now – about 3 million Americans undergo cataract surgery every year. It can be done at Milan Eye Center’s very own outpatient surgery center. Any eye surgery can stir up anxiety. But the realities of cataract surgery are sometimes surprising to patients:
After the procedure, vision may be slightly blurred with a mild foreign body sensation for the first few days. But, cataract surgery recovery is usually fast with many patients returning to normal day-to-day activities or work by the next day. Over 98% of patients obtain a significant improvement in vision after the cataract surgery procedure.
The benefits of cataract surgery go beyond improved vision and returning to normal everyday tasks. According to studies done by the American Academy of Ophthalmology, some patients also attain improved sleep, moods, and mental capacity.
During cataract surgery, an artificial lens or intraocular lens implant (IOL) replaces the natural lens of the eye. At Milan Eye Center, our expert surgeons offer the entire breadth of cataract surgery lens options to correct your vision.
Traditional implants typically provide good distance vision but often require the continued use of glasses or contact lenses.
Toric implants, patients can elect to not only have their cataracts removed but also correct astigmatism. (Watch Testimonial)
Multifocal implants give patients the opportunity to eliminate the need for glasses or contact lenses. (Watch Testimonial)
Though traditional cataract surgery is a medically covered procedure (bladeless is an additional cost), patients may have a choice of advanced technology IOLs to enhance their visual function after surgery. The different IOL choices have varied out-of-pocket costs. If you’re a candidate for any of the advanced IOLs, your surgeon will discuss their implications.
Milan Eye Center offers Healthcare Finance Direct (HFD). Unlike traditional lenders, HFD approves nearly all applicants regardless of credit score and does not conduct hard credit checks, ensuring no damage to the patient’s credit. This system makes treatments more accessible and alleviates the financial burden on patients, allowing them to focus on their healthcare needs without the stress of upfront costs.
Cataracts can be so gradual that you won’t immediately know there’s a problem. There is no pain associated with cataracts, and your brain has a remarkable ability to adapt to diminishing vision.
If you’re over the age of 50, you might have noticed a few changes in your eyesight in recent years. Early cataracts may not affect your vision or have a mild effect on the quality of your vision. But as they progress, you may notice a general “fog,” “smokiness,” or require more light to read. An increase in your glasses prescription may temporarily help improve your vision. However, as cataracts progress, your vision can continue to worsen. It may be time for cataract eye surgery when vision problems begin to interfere with your daily life. Any number of symptoms could dictate the need for cataract surgery, including:
An ophthalmologist will determine whether you have early signs of cataract development using what’s called a “dilated eye exam.” A magnifying lens will examine your retina and optic nerve for signs of damage and other eye problems.
Schedule a Consultation To Improve Your Vision Today
Three types of cataracts are: nuclear, cortical, and posterior subcapsular. Nuclear cataracts are graded according to their color and opaqueness. Cortical and posterior subcapsular cataracts are graded to the degree of interpupillary space obscured and the degree of posterior capsule obscured.
Different grading systems describe cataract severity; typically, labeling Grade 1 as Mild, Grade 2 as Moderate, Grade 3 as Pronounced, and Grade 4 as Severe.
These occur when the center of the eye (or “nucleus”) goes hard (or “sclerotic”) due to compression of older lens fibers in the nucleus by new fiber formation.
As the nucleus hardens, it becomes cloudy (or “opacifies”) and affects your vision. Nuclear sclerosis is the most common of the three. (Source: American Academy of Ophthalmology)
These occur when the outer layer of the lens (or lens cortex) becomes opaque. Over time, the clouding moves from the periphery of the lens cortex to the center, much like the spokes in a wheel.
People with diabetes are at more risk of developing cortical cataracts. (Source: Javadi, M.A., Zarei-Ghanavati, S.)
These are caused by opacities in the most posterior cortical layer, directly under the lens capsule. These cataracts are more common in younger age groups. They tend to form faster than cortical or nuclear sclerotic cataracts (with symptoms surfacing within the first few months). (Source: M. Edward Wilson)
Studies have also found that people taking steroids, have diabetes, or suffer from extreme nearsightedness and/or retinitis pigmentosa, are more prone to developing this type of cataract. (Source: Jobling A., Augusteyn R.C.)
Approximately one in four patients who have cataract surgery will develop cloudiness on the back of the newly implanted lens. Cloudiness generally occurs within 5 years after surgery, and there’s no way to predict who will develop it. If this happens, our physicians can easily correct the problem with an in-office procedure known as a YAG posterior capsulotomy. A surgical laser opens the clouded capsule, allowing light to pass through to the retina.
Fortunately for patients, this procedure is generally painless and completed in a matter of minutes. It can very quickly restore a patient’s vision after cataract surgery. Some floaters are normal after the YAG capsulotomy, but they should resolve within a few days. Then, the patient will return for a postoperative visit to ensure everything is looking good and vision has improved.
Our knowledgeable staff is here to answer all your questions about which procedure is best for you, and ensure you have the most comfortable experience possible. Make an appointment today at one of our eight convenient locations.
Schedule an Appointment Online
Or call 678-381-2020